Infection and Your Joint Replacement
An infected hip or knee replacement represents a very important problem for both you and your surgeon.
An infected hip or knee replacement represents a very important problem for both you and your surgeon. Currently, infection is the most common reason for revision knee replacement surgery and the second most common cause for revision hip replacement https://aaos.org/registries/registry-program/american-joint-replacement-registry/. Infections may develop shortly after joint replacement surgery or years later. On average, the risk of developing an infection in the United States from a first-time joint replacement is approximately 1-2% and 4-5% after a revision surgery. Certain factors have been identified which increases your chances of infection including length of surgery and your personal medical issues.
Research has shown that good control of your chronic medical issues and other risk factors can significantly reduce your risk of infection. If an infection does occur, it is important to act promptly in attempt to salvage your joint replacement and prevent the infection from spreading to other parts of your body. Most joint infections CANNOT be adequately treated with simple oral or intravenous antibiotics.
Printer Friendly
Click to print
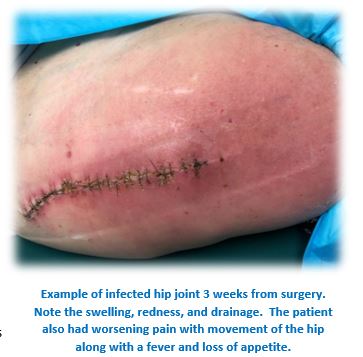
What are Signs and Symptoms of Infection?
Infections present differently among patients. Obvious infections may present with continuous pain, swelling, drainage, and redness while others may only complain of a dull ache or persistent stiffness in their joint. Any abnormal pain in your replaced hip or knee should be concerning, especially pain that does not go away with rest. Although occasional redness or warmth around the joint can be expected for up to 1 year after surgery, persistent or worsening signs including unexplained or an rapid increase in swelling may signal infection. In addition to pain at your joint, symptoms such as fever, chills, or sweats may signify infection. Prolonged wound drainage (more than 3 days) immediately after joint replacement surgery may increase your risk of infection according to recent studies. It is important to promptly communicate with your surgeon if any of these signs or symptoms arise.
Occasionally a fluid (seroma) or blood collection (hematoma) may form under the incision early in the recovery period. These collections can risk an infection developing. As a result, your surgeon may have to “drain” or “wash-out” the area to help prevent or treat a joint infection.
If your incision begins to look suspicious, it is a good idea to let your surgeon know as soon as possible. Sometimes the incision can break down due to an irritating stitch but other times an opening in the incision can signify an underlying infection. The former can usually be treated with local wound care while the latter will likely require a trip to the operating room.
Checking for Infection?
It is very important to contact your surgeon if your hip or knee joint does not feel right. If an infection is suspected, your surgeon will usually obtain X-RAYS, BLOOD WORK, and possibly a SAMPLE OF FLUID from your affected joint. The blood work is usually analyzed for inflammatory markers which become elevated during an infection while the joint fluid is analyzed for bacteria particles and other markers which may signify infection. It is important for your doctor to identify the infection and the bacteria causing it before antibiotics are started.
What Happens During an Infection?
Most infections are caused by BACTERIA, or rarely a YEAST (FUNGUS), that evades your immune system and causes inflammation and irritation around your hip or knee joint. Infections usually occur at two time periods: ACUTE and LATE.
- ACUTE (within 4-6 weeks of surgery): An acute infection is usually the result of something around the time of surgery. Your joint replacement is exposed to the outside environment during surgery and the normal skin barrier is disrupted, presenting the perfect opportunity for bacteria to sneak into your incision. Thankfully, surgeons take extra precautions to decrease the chances of developing an infection. Ensuring your medical issues are optimized prior to surgery, intravenous antibiotics during surgery, special skin washes, wound irrigation during surgery, minimizing blood loss, and special dressings after surgery all do their part to help limit your chance of infection. Therefore, it is very important for the incision to heal as quickly as possible to re-establish a barrier to the outside environment.
2. LATE (6 weeks or more after surgery): Most infections occur weeks to months after surgery. Late infections are usually spread through the bloodstream from another part of the body. For instance, a urinary tract infection or tooth abscess may lead to an infection in your joint replacement(s). We encourage patients to maintain regular follow-up with their surgeon and primary care physicians to maintain good health status. Several theories suggest that as we age our immune system weakens and occasionally bacteria can travel through the bloodstream and hide in a replaced joint. An infection may also hide in the joint, but only appear later as a late infection.
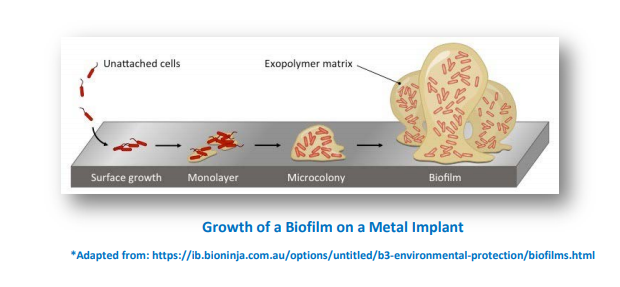
Once bacteria reach your hip or knee implants, they stick to the surfaces and start producing a slime layer called a BIOFILM which helps shield them from your body’s immune system and most antibiotics. According to research, it takes about 3 WEEKS for the biofilm to fully develop. Once the biofilm is mature, it is very difficult to defeat the bacteria without surgery to remove the implants and clean the tissues around the joint.
This is why it is very important that you pay close attention to your new hip or knee joint. If an infection is caught early, your surgeon may be able to salvage your implants and thoroughly wash the implants to remove the biofilm. Delayed treatment may require that the implants be removed for a short time before new implants are inserted. Current research is investigating different ways to stop the biofilm from forming and how to break up the biofilm without having to remove the implants.
What are the Treatment Options?
If the infection is caught early (within 3-6 weeks of surgery/symptoms), a “washout” procedure can be performed where the infected joint is opened in the operating room, the infected tissue is debrided (i.e. cleaned), and the joint is thoroughly washed along with exchange of modular pieces (the plastic spacer in knees or the ball and liner in hips Implants | Hip and Knee Care (aahks.org). The implants are left in place if secured to the bone. After surgery, intravenous antibiotics are prescribed for about 6 weeks to help your immune system fight the infection. Sometimes, oral antibiotics are necessary for several months or years after some of these procedures.
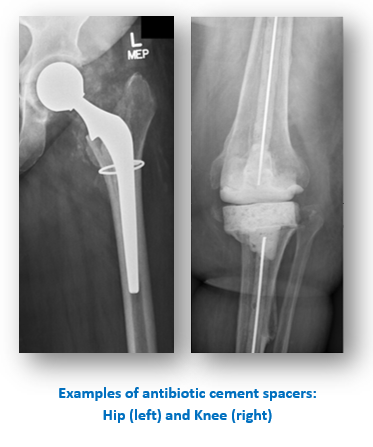
For infections discovered after 6 weeks of symptoms, it becomes more difficult to clear an infection because a biofilm has had enough time to form. At this stage, the most frequently used treatment in North America is a TWO- STAGE REVISION surgery. All the implant components may need to be removed for a short period of time to give you a better chance to clear the infection. In this setting, a temporary implant is inserted for several weeks followed by intravenous antibiotics until another new implant can be inserted (also known as a two-stage exchange procedure). This temporary implant may be custom made in the operating room from cement. Alternatively, the implants can be removed and all reinserted in the same surgery, called a One-stage procedure. Studies are currently underway comparing the outcomes of One-stage vs. Two-stage procedures. Your surgeon is in the best position to guide you through this decision-making process.

During a 2-stage procedure your surgeon will likely place a cement spacer impregnated with antibiotics to attack the infection from inside the joint. An infectious disease physician is usually consulted to help decide which intravenous antibiotics and dosages are best to treat your infection. Some of the antibiotics used to treat the infection need to be monitored to ensure they do not overtly harm your kidneys or liver. Therefore, it will be important to follow up with your infectious disease specialist and your surgeon.
Most patients with an infected joint replacement are able to undergo the second stage of the revision surgery, but unfortunately there are some patients who are too sick or have been diagnosed with a difficult to treat bacteria/yeast that limits their abilities to undergo the second stage surgery. Lastly, the mortality (chance of dying) of an infected joint replacement has been found to be higher than some common cancers at 5-years, highlighting the importance of proper identification and management of an infected joint replacement.
How to Lower the Chance of Infection?
Having an experienced surgeon and staff is integral to the overall success of your joint replacement. No one asks for a joint infection but unfortunately, they do occur. Recovery after an infection is usually more difficult than your first joint replacement. Like any revision joint replacement surgery, it will take time to regain your motion, strength, balance, and endurance. You can expect to begin to resume more normal activities about 3-4 months after revision surgery for infection, if successfully treated.
Remember, recovery after an infected joint replacement takes a team approach including your friends and family, nurses, therapists, medical doctors, and surgeon. Addressing your risk factors BEFORE surgery is the first step to lowering your chance of infection AFTER surgery. Several studies have been performed researching optimizing medical conditions prior to surgery to decrease your chance of infection. Some of the biggest contributors to infection include uncontrolled diabetes, a prior infected wound/joint, smoking, and obesity. Others include dental issues, kidney disease, autoimmune diseases, liver disease, and heart issues. Infection | Hip and Knee Care (aahks.org) Remember, it will be important to keep a healthy diet (protein, dairy, leafy green vegetables) to help your body take in the necessary building blocks to both heal and prevent infection after surgery. Research continues to investigate new ways to prevent and treat infected joint replacements.
Conclusion
The average risk of infection after a hip or knee replacement is between 1-2%. Great care is taken to prevent infection before, during, and after surgery. As a joint replacement recipient, you should be on the lookout for symptoms of an infection: persistent joint pain with swelling, warmth, drainage, and redness with or without fevers, chills, or sweats. Any change in the function of your replacement should prompt a call to your surgeon for further advice. Early treatment can help to preserve your joint replacement. Above all, most joint infections CANNOT be adequately treated with simple oral or intravenous antibiotics.
These articles have been written and peer reviewed by the AAHKS Patient and Public Relations Committee and the AAHKS Evidence Based Medicine Committee. Links to these pages or content used from the articles must be given proper citation to the American Association of Hip and Knee Surgeons.


